A Systematic Evaluation of Immune Response and Plaque Microenvironment Variation in Alzheimer’s Disease
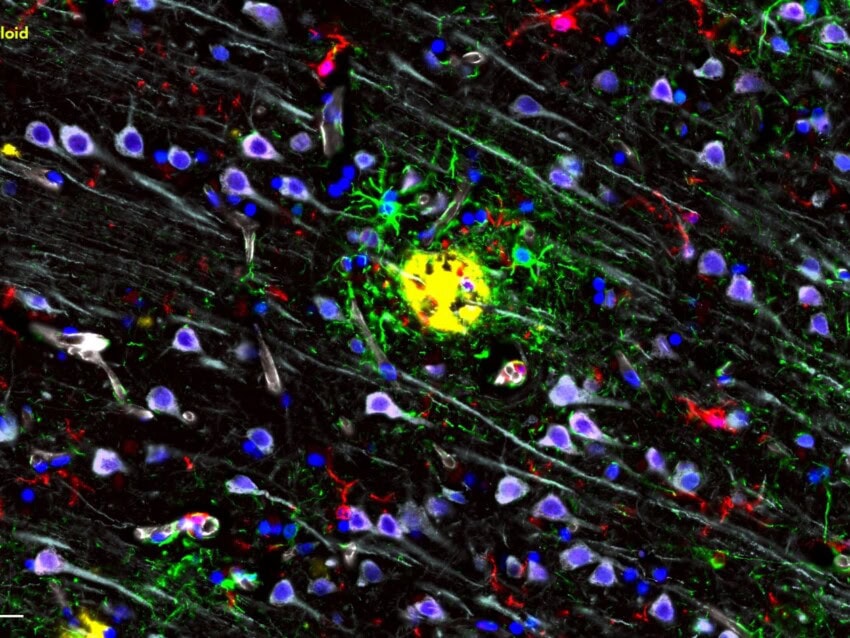
Alzheimer’s disease (AD) – the most prevalent form of dementia – is associated with defining histopathological features that include amyloid-beta (Aβ) plaque deposition and tau protein aggregation, accompanied by synaptic loss, neuronal death, and cognitive decline. The neuropathological changes in sporadic, late-onset AD are believed to be modulated by innate immune cells of the central nervous system, primarily microglia. While microglia have a well-established disease-modifying role through Aβ phagocytosis and pro-inflammatory cytokine production, their precise contribution to disease pathogenesis remains poorly understood. A multimodal analytical study conducted by Prokop et al. highlights the complex role of central nervous system immunity in AD by investigating the variability in microglial phenotype, morphology, and function as well as amyloid plaque microenvironment across patients and brain anatomical regions.
The authors observed an increase in activated microglia with progressing Aβ and tau pathology and with AD-associated genetic risk variants (R47H and R62H) in the triggering receptor expressed on myeloid cells 2 (TREM2). The activation of microglia was reliant upon co-occurring protein aggregates. This order of events suggested that protein accumulation induces neuronal damage and an immune response cascade that in turn modulates their toxicity and progression in AD. While dystrophic microglia exhibited a similar increase in later stages of the disease, their abundance was more pronounced in TREM2 variant carriers. This led the authors to speculate that sequence variations in TREM2 are responsible for altering the functional state of microglia with respect to chronic activation due to accumulated neuropathology in late-stage AD.
Further evaluation of the impact of TREM2 variant carriers demonstrated a concomitant reduction in microglial clustering around plaques and an elevation in insoluble phosphorylated tau. The authors postulated that TREM2 mutations can contribute to an increase in plaque neurotoxicity and neuritic dystrophy. They attributed that to a disruption in the microglial neuroprotective barrier that typically regulates amyloid compaction and limits fibril outgrowth. The impact of TREM2 variants extended beyond changes in phosphorylated tau protein levels. Using the NanoString GeoMx™ DSP platform, high multiplex digital spatial profiling of 40+ protein targets also revealed altered plaque microenvironment composition in TREM2 variant cases.
Transcriptomic analysis was then pursued to corroborate immunohistochemical findings and further elucidate pathophysiological pathways underlying late-onset AD. Using NanoString’s nCounter® Human Neuroinflammation and Neuropathology panels, the authors demonstrated significant differences in the expression profile of functionally-relevant gene sets between anatomical regions of high neuropathology AD patients with and without TREM2 variant expression. TREM2 variant cases exhibited a downregulation of microglial and astrocytic activation in the visual cortex, an upregulation of pro-inflammatory processes in the frontal cortex, and mixed immune response patterns in the hippocampus, suggestive of differential responses due to the respective brain region-specific disease stage.
Altogether, study findings underscore the complementarity of analytical techniques in investigating multifactorial and heterogeneous biomedical disorders. By adopting a systematic approach – through integrated immunohistochemical characterization of morphology, spatially-resolved and high-plex quantification of protein expression, and pathway- and cell-type specific gene expression analysis – the authors were able to provide a unique insight into the complex pathogenic interactions between the innate immune system and plaque microenvironment in late-onset AD.
Watch Comprehensive analysis of microglia across neuropathological stages of Alzheimer’s disease (AD)